Who doesn’t have a smartphone this day and age? Therefor a plethora of health apps are available for all kind of issues. But as a health scientist and pelvic physiotherapist ofcourse I want to know all about…the evidence. A few years ago I presented at a conference about the use of apps and the evidence regarding the effectiveness for treating urinary incontinence. However, effectiveness of a treatment app is one thing but the willingness to use an app is another. The research I will discuss today adds to our knowledge about the use of a treatment app for urinary incontinence.
Women who had visited their general practitioner for their urinary incontinence in the past 10 years were invited to participate in face-to-face interviews. They also had to report urine loss of at least 2 times a week, a willingness to get treatment and access to a smartphone or tablet.
Nine women were interviewed about their user experience and preference regarding an app for the treatment of urinary incontinence. They were aged between 32 and 68 years, had different types of urinary incontinence and duration of symptoms and moderate to high self-reported eHealth literacy.
Previously, six of the nine women had been treated by a pelvic physiotherapy and one with medication. The women used the app for 6 weeks. The app discussed in this research covers: stress-, urgency-, and mixed urinary incontinence. The app uses advices and pelvic floor muscle training described in the guidelines (for general practitioners) for treatment of urinary incontinence in The Netherlands.
RESULTS
Four themes emerged from the interviews (Table 1).
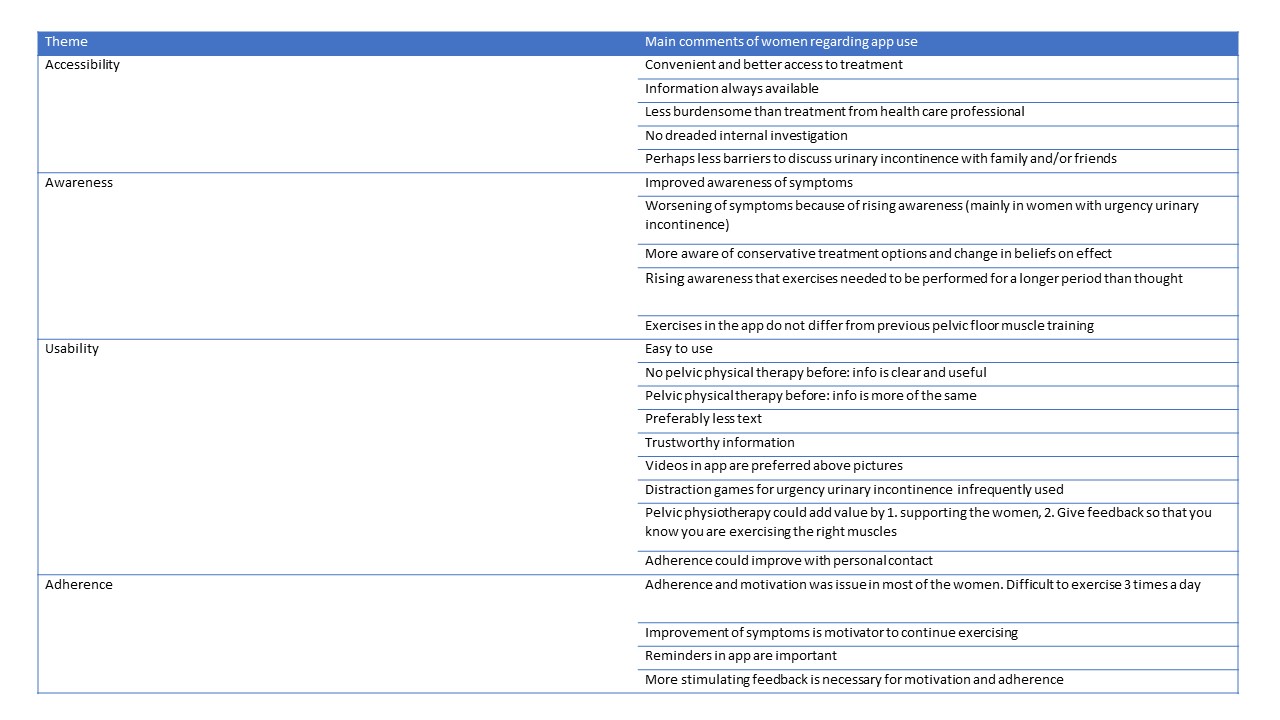
The results show that adherence to the app was not great by the participating women. The authors state that this doesn’t mean that the women didn’t exercise. Maybe they exercised without using the app all the time. In the discussion of this article it was mentioned that research regarding adherence to apps has shown that adherence is low without face-to-face contact.
Last but not least. This research was performed in a part of The Netherlands so generalizability is compromised.
BOTTOM LINE (PERSONAL THOUGHTS)
This research shows that among other things face-to-face contact with a health professional (pelvic physiotherapist) an app, and the reminder function in an app is valued by women. We know that quite a lot of women don’t know how to contract their pelvic floor muscles properly, so good instruction is very important.
So will a combination of pelvic physiotherapy with assistance of an app have better results than pelvic physiotherapy, or an app alone for the treatment of urinary incontinence? I know that at the moment research is done regarding an app (iPelvis) that is specially designed to use in combination with treatment by a pelvic physiotherapist. This research might answer my question in the future. I look forward to the results and will keep you posted!
Reference:
Wessels NJ, Hulshof L, Loohuis AMM, van Gemert-Pijnen L, Jellema P, van der Worp H, Blankers MH. User Experiences and Preferences Regarding an App fort he Treatment of Urinary Incontinence in Adult Women: Qualitative Study. JMIR Mhealth Uhealth 2020;8(6):e17114.









Recent Comments